Address cardiovascular disease with both new technology and well-known advice.
by Cassie Richardson
Imagine if preventing a heart attack was as easy as swallowing a pill.
The idea may sound like an imaginary convenience taken straight from the Space Age world of cartoon character George Jetson. But at Google X, Google's semi-secret research facility in Mountain View, Calif., scientists are working to bring this concept to reality.
Google researchers believe in the possibilities of a pill containing nanoparticles–tiny protein-coated molecules capable of detecting other molecules with specific biomarkers–that can help spot cardiovascular disease and other health conditions at very early stages, even before noticeable symptoms appear.
Here's how Google X researchers believe their conceptual pill can work: A patient swallows the pill containing thousands of magnetic nanoparticles. As the pill is absorbed by the body, these tiny particles enter the bloodstream and travel throughout the body, collecting clues about the patient's cardiovascular health. In the doctor's office, a small device worn on the patient's wrist, similar to a watch, may be used to attract the magnetic particles and then interpret the information gathered from blood vessels throughout the body.
“It sounds like something from ‘Star Trek,'” says Daniel Linert, M.D., an interventional cardiologist with Porter Regional Hospital Physicians Group. Yet the need to save lives by detecting cardiovascular conditions early, before a stroke or a heart episode, is more reality than science fiction.
In most cases, men and women discover they have cardiovascular troubles during an emergency room visit to find relief from symptoms. According to the American Heart Association, three men out of every thousand will have their first cardiovascular event between 35 and 44 years old. This rate increases dramatically with age–74 out of every thousand men between 85 and 94 years old will see the first visible symptoms of cardiovascular disease. The rates are similar for women, though the first cardiovascular event typically appears 10 years later than in men.
While scientists continue to explore new techniques for addressing one of the nation's top health concerns, Dr. Linert says determining the likelihood of future heart attacks or strokes is quite possible, today. “What we've been using over the last several years has been working for us about cardiovascular disease and risk factors for cardiovascular disease.”
Dr. Linert says annual blood tests that evaluate blood count, lipid profiles and thyroid hormones work well to detect cardiovascular disease. On the other hand, determining the risk for heart attack and stroke can be as simple as understanding the patient's health history and lifestyle habits. Age, weight and a history of heart disease, diabetes, chronic obstructive pulmonary disease, high blood pressure, high cholesterol, kidney disease or anemia can all signal possible heart problems. Smoking, alcohol consumption and frequency of exercise are important factors as well.
Still, the nanoparticle pill technology's potential for identifying traces of fatty plaques in blood vessels that could lead to heart attack or stroke, and pinpointing cardiovascular issues much sooner than existing tests, should come as exciting news for people of all ages–including the 42.2 million Americans over age 60, who have one or more types of cardiovascular disease.
“That field [of nanoparticles] is kind of interesting,” says Jagdeep Sabharwal, M.D., an interventional cardiologist with Beacon Health System in Elkhart. For years, medical researchers have reveled in the promise of similar technologies for detecting and treating cancer, so the idea of applying this technology to detect very early cardiovascular disease and prevent heart attack is intriguing. Yet “I think we're a long ways from it.”
In his practice, Dr. Sabharwal uses relatively simple, tried and true tests to detect coronary disease and, hopefully, prevent heart attacks in his patients' near futures. These commonly-used tests include electrocardiogram (EKG), which measures heart electrical activity, and stress testing, which monitors heart rate at periods of rest and exercise.
“Things are relatively simple: There is no miracle genetic testing that's going to tell us and reduce the risk of heart attack for the elderly,” Dr. Sabharwal says.
“I'm an interventionist. I do some plumbing work. I can open up the blockages, but what has a more long-lasting effect are these five things that help in prevention of heart disease and heart failure,” Dr. Sabharwal says, adding that no pill or technology can replace or trump the impact of the following lifestyle changes:
* Eat a healthy diet that contains fruits, vegetables, nuts, reduced fats in dairy products, whole grains and fish, to reduce risk of heart attack by about 15 percent.
* Enjoy a glass of wine or small alcoholic beverage (10 – 30 grams a day) and reduce risk of heart attack by 11 percent.
* Quit smoking and reduce your risk for heart attack and stroke almost three- to five-fold.
* Regardless of your age and mobility, do some form of aerobic exercise. This can reduce your risk of heart attack by 3 percent.
* Lose weight and keep a trim waistline to reduce your chances of having a heart attack by approximately 17 percent.
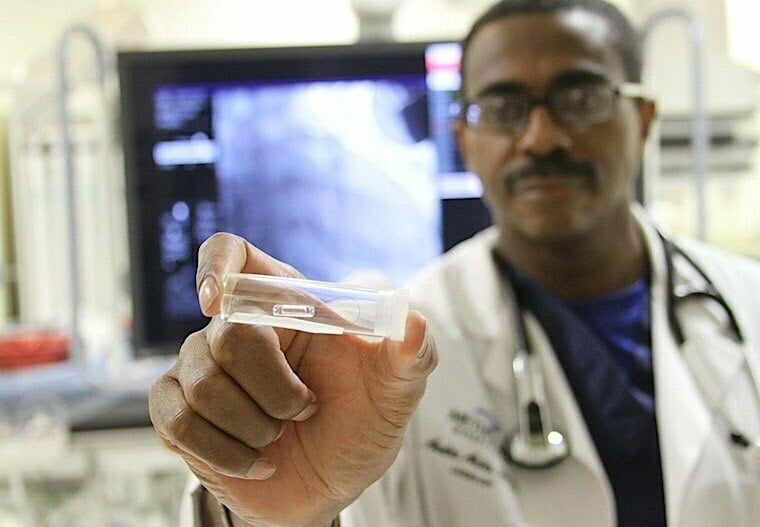
Though the nanoparticle technology is still on the horizon, some amazing devices are realities today. One groundbreaking new technology is the CardioMEMS HF System, which is providing patients of Northwest Indiana's Methodist Hospitals a better chance of survival following hospitalization. Among patients in this age range who have been hospitalized for heart failure, there's a 20 percent change of an unexpected return to the hospital–or even death–in the month following their discharge from the hospital.
CardioMEMS is a tiny, wireless implant that cardiologist Andre Artis, M.D., uses to remotely monitor patients while they recover at home. Methodist is the first institution in the region to offer the FDA-approved heart-monitoring device. Studies have shown that CardioMEMS can reduce mortality significantly, and cut the rate of heart failure hospitalizations.
Another technology that might blossom sooner than nanoparticles is genetic testing that will allow physicians to prescribe medications based on each cardiovascular patient's unique biochemistry.
“I can very well see that a similar type of [pill] concept can be developed, and information can be obtained for the clinician as to the patient's predisposition and or risk for various cardiovascular disease states,” says Paul Jones, M.D., Franciscan Health System medical director of cardiovascular services.
For example, there are many blood thinner and anti-hypertension medications on the market. And in many instances, health care workers use their best judgment to make sure the right patients receive the most effective prescriptions. This is because everyone is different. Therefore, not every patient will respond in the same way to the same medication.
“Technology does not surprise me,” Dr. Jones says. That's because several new and cutting-edge technologies are available to help cardiovascular experts bring new options and better outcomes to their patients, especially elderly patients who, typically, are considered poor or risky candidates for conventional, open-heart surgical procedures.
“Some of the advances in technology that we use today, and we will be using even more so tomorrow, that have revolutionized how we care for our patients” are related to “the advent of non-surgical catheter treatment strategies for cardiac and particular vascular disease,” Dr. Jones says. “There's major, major progression in that area.”
At Franciscan Health System, patients–such as one very active 92 year-old whose physician believed repairing a very large aortic aneurysm with conventional surgery and general anesthesia was too risky–are finding new hope with an advanced technology known as percutaneous endovascular repair of aortic aneurysm. With this newer technique, most patients return home 23 hours after treatment.
Transcatheter aortic heart valve replacement (TAVR), which Dr. Sabharwal offers in his practice, is another lifesaving treatment that is saving the lives of elderly patients who are considered too frail or too old to withstand conventional heart valve replacement surgeries. This technique, which received FDA approval in 2012, allows surgeons to replace a diseased heart valve with an artificial one, through the groin. The conventional open-heart valve replacement surgery is much more invasive.
“The recovery is much faster and patients who would have a very difficult time recovering from a traditional open heart surgery, they do pretty well with this,” Dr. Sabharwal says.