Technology boosts speed and accuracy of treatments.
by Laurie Wink
Area hospitals and medical practices are using leading-edge approaches to diagnose and treat cancer patients. By harnessing the power of the latest high-tech tools, physicians are significantly improving the speed and accuracy of cancer treatments and reducing the pain and discomfort of patients during medical procedures.
Cancer continues to be the second leading cause of death in the United States, after heart disease. More than 1.5 million people were diagnosed with cancer in 2011 and more than 575,000 people died, according to the United States Cancer Statistics report. The World Health Organization reports 14 million people worldwide are diagnosed with cancer each year, and about 8.2 million die of the disease.
The good news is that two out of three people who are diagnosed with cancer are surviving five or more years, according to a study released this year by the Centers for Disease Control and Prevention. Advances in cancer detection and treatment methods are improving the odds of survival for cancer patients. And new technology is making it possible for cancer specialists to plan and deliver personalized patient care using research-based best practices.
An innovative approach to treating cancer with image-guided radiotherapy is now being used at St. Mary Medical Center in Hobart. The hospital recently invested $4.5 million to acquire TrueBeam(TM), an advanced medical linear accelerator that significantly improves radiation treatment for patients with lung, breast, prostate, head and neck cancers.
Radiation oncologist Dr. Koppolu Sarma says TrueBeam is a faster, more accurate treatment delivery system. “More patients are being cured with this technology and having fewer side effects because it delivers more of the dose to targeted areas and avoids doses to normal organs,” he says. “It makes delivery much easier.”
TrueBeam produces a 3-D image of the tumor and uses computer technology to compensate for patient movement during treatment. This is important, Sarma notes, because it reduces the chances of damaging surrounding healthy tissues. Truebeam produces multiple beams programmed to the exact shape of the tumor, resulting in more accurate doses.
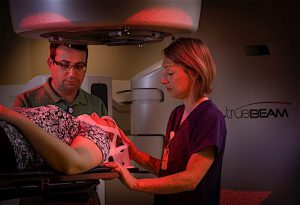
Using the Vision RT infrared guidance system to setup a patient to receive Stereotactic Radiosurgery on the Varian Truebeam linear accelerator.
And TrueBeam treatments are ten times faster. Instead of 20 minutes for a standard radiation treatment, TrueBeam takes two minutes. Sarma says the faster treatment time is particularly helpful for older patients who find it hard to lie still.
At Memorial Hospital in South Bend, another advanced radiation therapy technology is being used to treat brain cancer patients. VisionRT (AlignRT(R)), an optical guidance technology, is making it more comfortable for patients to undergo Stereotactic Radiosurgery (SRS) treatments, according to Dr. David Hornback, radiation oncologist and medical director of radiation oncology at Memorial Hospital.
“VisionRT is a safe, accurate motion management tool that increases patient comfort, “Hornback says. “Memorial is at the leading edge of using technology that is rapidly taking over as the procedure of choice.”
He explains that SRS uses precisely focused radiation beams to treat tumors in the brain, neck and other parts of the body. The standard procedure relies on a painful metal head frame, or halo, that is clamped onto the skull to keep patients motionless. The head frame is then clamped onto the treatment table during a CT scanning process and subsequent radiation treatment.
“It's uncomfortable,” Hornback says. “Oftentimes, depending on the location of the tumor, you would get a little bleeding and bruising, and some headaches. Now, with the VisionRT optical 3-D mapping technology, patients are immobilized with a custom-made, rigid, open-faced mask. The optical guidance cameras use surface rendering technology to aid in accurate setup and delivery of precise treatments. What we're doing is delivering very high doses of radiation with less than a millimeter margin for error. If a shift of even 1/8 inch occurs, we're treating normal tissue. The precision part of this is extremely, extremely important.”
SRS is most commonly used to treat small tumors–from 1/8 of an inch up to 2 inches–in patients whose cancer has metastasized to the brain. Hornback says the treatment is determined by the number of tumors in the brain.
“If there's a significant number, we do whole brain radiotherapy. But there can be side effects, including memory and calculation problems and fine motor movements. In general, we're comfortable treating up to four spots on the brain to avoid whole brain radiation.”
The VisionRT optical tracking system hasn't changed SRS treatment, but it has improved the accuracy of treatment and patient comfort. Hornback cites the example of a woman who had SRS treatment two years ago and needed further treatment because a small spot showed up.
“She had the option of going ahead with treatment using the head frame or waiting for the new technology to be offered,” he says. “She had such an aversion to having the head frame put on that she decided to wait. She was sold (on VisionRT) in an instant. The difference was fantastic to her.”
Porter Regional Hospital in Valparaiso is the first hospital in Northwest Indiana to use magnetic resonance imaging (MRI) technology to help diagnose prostate cancer. MRI is being fused with a traditional ultrasound exam to allow physicians to view previously undetected growths and perform targeted biopsies. Called “multiparametric MRI,” the new approach is becoming the standard for diagnosing and treating patients at various stages of prostate cancer according to Dr. Vivek Mishra, interventional radiologist and chair of the Department of Radiology at Porter Regional Hospital.

“MRI gives an exquisite amount of details of the prostate and fairly accurately pinpoints the cancer,” he says. “It's becoming more mainstream.”
Interventional radiologists work in tandem with urologists to determine whether or not MRI results are suspicious. When MRI images are fused with ultrasound images, urologists are able to perform targeted biopsies and detect prostate cancer more accurately, Mishra says.
The ability to produce a more accurate picture of a patient's prostate cancer is significant, Mishra notes, because it's currently the second leading cause of cancer deaths in men in the United States. The National Cancer Institute predicts that some 220,800 new prostate cancer cases will be detected and about 27,000 men with prostate cancer will die in 2015. More accurate diagnostic tools are leading to early detection and improving the odds of survival.
“Those with prostate cancer typically don't die from prostate cancer,” Mishra says. “They die with prostate cancer.”
Michiana Hematology Oncology (MHO), a medical oncology practice with comprehensive cancer centers throughout Northwest Indiana, South Bend and Mishawaka, is using CancerLinQ(TM) to improve care for patients with all kinds of cancer. CancerLinQ is a new health care information system developed through the American Society of Clinical Oncology (ASCO), a nonprofit physician group focused on improving the quality of care for cancer patients.
Dr. Robin Zon, a medical oncologist with MHO, has been an active committee member and board member for ASCO. Through her involvement, MHO was selected as one of the first 15 oncology practices in the world using CancerLinQ.
She says, “It's a high honor to be one of the selected practices in the world using CancerLinQ. We're a vanguard practice.”
Zon says oncologists have difficulty keeping up with the rapidly growing research findings about cancer patient care. And most of what is known about best practices is based on a small number of patients who participate in clinical trials. Of the nearly 1.7 million people in the United States who are diagnosed with cancer each year, only about three percent enroll in clinical trials that are required for FDA approval of new cancer treatments.
“They are not necessarily typical of patients we see in the office,” Zon says. “All of these years, we've based treatments on patients who don't look like the patients in front of us. And all of the information about outcomes for patients is hidden away in files. If, for example, I have an 82-year-old patient who is vital but has cancer and wants to know how similar patients have done, I can't readily answer that question.”
CancerLinQ allows Zon and other oncologists to enter data on an individual patient during an appointment and find out immediately how that patient compares to those with similar parameters and what treatment plans have produced the best outcomes.
“CancerLinQ is a new universe of practical insights,” Zon says. “It reassures me and my colleagues that what we're recommending is the best possible, evidence-based treatment. And it also reassures patients that they're getting the best care based on others like themselves.”
As knowledge of the genetic components of disease expands, medical researchers are finding that cancer is a complex disease that takes many different forms. For example, Zon explains, “In the past, we thought there were only a few types of lung cancer. Now we know that there are many different kinds.”
CancerLinQ helps physicians cut through the complexity and come up with more targeted treatments. “It increases the chances that treatment will work and decreases chances of unnecessary side effects,” Zon says. “And it's helping (health care) payers by not wasting money on treatments that have no chance of working. All the stakeholders are winners.”
Because of advances in diagnosis and treatment of cancer, more than 15 million people have survived cancer, but about one third of them continue to experience pain after treatment, according to Dr. David Miller, director of interventional and comprehensive pain management for Indiana University Health. Miller heads a team of pain management professionals at the IU Health Lifeworks Facility in Michigan City, the only comprehensive pain management center in Northern Indiana.
The term “cancer survivor” generally refers to those who have not been on active treatment of their cancer for several years, Miller says. Most cancer survivors get pain relief through a combination of treatments–which can include medications, physical and massage therapy, acupuncture and chiropractic treatment. But about 10 percent continue to have pain.
“It turns out a lot of chronic cancer pain in patients [that] I take care of is the residual result of permanent nerve injury,” he says. “The pain I deal with is not responsive to over-the-counter pain relievers or prescription pain meds.”
Miller is a board certified specialist in pain management with 25 years of experience in treating patients who have permanent nerve injury pain, called neuropathy. When other pain treatments aren't effective, Miller uses spinal cord stimulation, which he compares to “a pacemaker for the nerve.” The technique involves inserting a lead wire into the spinal canal and connecting it to a battery-powered pulse generator implanted under the skin. The device sends electrical signals into the spinal cord and changes the way pain information is processed.
Spinal cord stimulation has been used for more than 30 years but has had one major drawback. “When the stimulator was turned on, a patient would feel a tingling or prickling sensation in the area of the nerve being stimulated,” Miller says. “Many patients would not find those sensations to be pleasant.”
Recent advances in the technology are making it a more widespread pain treatment for cancer survivors, according to Miller. Now, with brief bursts of higher frequency signals, patients are getting better pain relief and are no longer feeling the unpleasant sensations during the spinal cord stimulation process. New stimulators have batteries that can be recharged through the skin and are smaller, lighter and more durable, he adds.
“Cancer-related pain is associated with depression, poor functioning and disruption of relationships with friends and family,” Miller says. “Reduced pain is important for their quality of life.”
One obstacle to expanded use of spinal cord stimulation to treat cancer pain has been the cost, Miller says, but recent studies have shown the treatment to be cost-effective in the long run, since many patients are able to stop taking medications and reduce the number of doctor visits.
Most cancer pain sufferers Miller sees are in their 70s and 80s and he says treatment can be complicated by the presence of other pain associated with the aging process. The likelihood of getting cancer increases with age.
“A lot of people have the notion of cancer as a young person's disease because of stories on TV and movies,” Miller says. “But incidents of cancer are more likely as we age.”
Some researchers believe that continued improvements in cancer treatment and prevention could significantly reduce deaths from cancer for people in most age groups. Scientists at the University College London and Kings College London predicted in a report released in January that most cancer related deaths in children and adults up to the age of 80 could be eliminated by 2050. They base the prediction on the fact that more people today are aware of cancer symptoms and are visiting doctors who are diagnosing the disease at earlier stages.
Although there is no one-size-fits-all approach to fighting cancer, medical professionals believe that rapid advances in our understanding of its causes, and methods of diagnosis and treatment, are allowing us to gain ground in the battle.
